World Kidney Day (WKD) is a joint initiative between the International Society of Nephrology and the International Federation of Kidney Foundations aimed at raising awareness of the importance of kidney health and reducing the impact of kidney disease. This year, WKD is Thursday 10 March, with hundreds of events all over the world [1].
Since the inaugural WKD in 2006, each campaign has had a specific theme. The theme for 2022 is [1]:
Kidney Health for All: Bridge the knowledge gap to better kidney care
Despite the widespread prevalence of kidney disease, a knowledge gap is evident in the general public, as well as among healthcare professionals and policymakers. Consequently, individuals may be unaware of the signs of kidney disease and the measures needed to maintain kidney health, and kidney disease remains a low priority for public health officials [2].
What is chronic kidney disease?
Chronic kidney disease (CKD) is the gradual decline in kidney function; it is a long-term condition that develops over months and years and is usually seen in older adults [3]. Anyone can develop CKD, but it is more likely in certain ethnic groups, such as Black or South Asian populations [3, 4]. It affects an estimated 1 in 10 people worldwide and is projected to be the fifth leading cause of death globally by 2040 [2].
A reduction in kidney function means that blood is not filtered properly, resulting in an excess of certain substances and accumulation of toxins in the blood [5]. It can also lead to water retention, which can increase blood pressure and damage the kidneys further. CKD is associated with other health problems, most notably cardiovascular disease; patients with CKD are at an increased risk of suffering from a stroke or heart attack [5, 6].
The rate of decline in kidney function varies among individuals. Some patients progress to kidney failure, where kidney filtration declines to such an extent that treatment is required to replace the lost kidney function (renal replacement therapy) [6]. However, out of the 3 million people currently with CKD in the UK, it is approximated that only 2% are receiving treatment for kidney failure [4]. The majority of cases are mild to moderate, and patients receiving the correct treatment are able to successfully manage their condition for many years [3, 6].
What causes CKD?
The cause of CKD varies. In most cases, several factors combine to put excessive strain on the kidneys, which leads to damage [3]. The two main risk factors for CKD are hypertension and diabetes; high blood pressure can damage the filtration units of the kidneys (called the glomeruli), and diabetes can damage blood vessels in the kidneys. This combines to reduce filtration and further increase blood pressure [6].
Other conditions that may contribute to CKD include [6, 7, 8]:
- Glomerulonephritis (inflammation of the kidney)
- Polycystic kidney disease
- Infection
- Long-term use of certain medications (e.g. non-steroidal anti-inflammatory drugs [NSAIDs])
- Obstruction to the flow of urine (e.g. due to kidney stones, an enlarged prostate or a tumour)
What are the symptoms of CKD?
The early stages of CKD are often asymptomatic, with symptoms typically manifesting when the disease becomes more severe (Stage 4); consequently, patients may not be diagnosed until the later stages [3]. If symptoms are present, they are typically non-specific and may include [3, 6]:
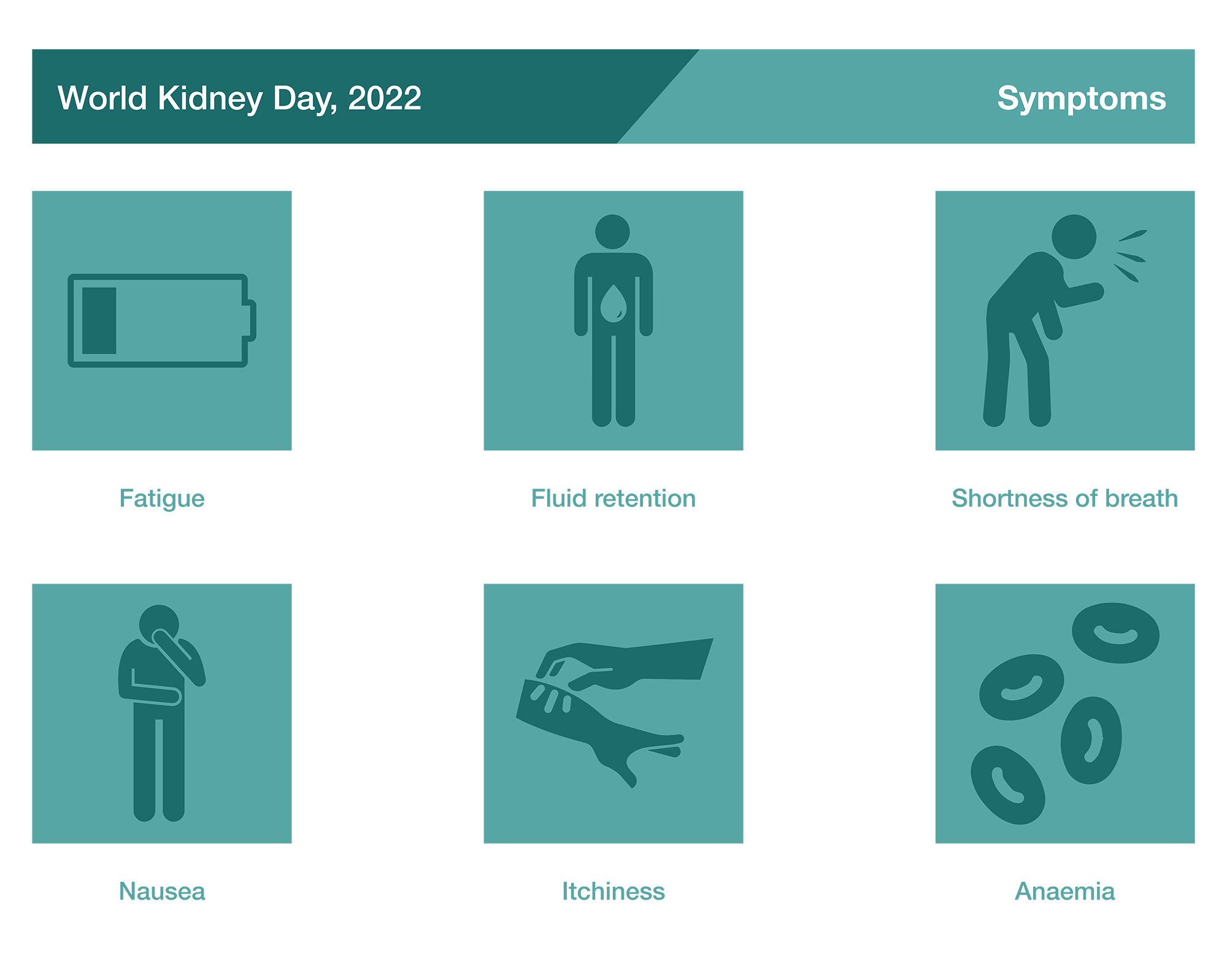
How is CKD diagnosed?
CKD is usually diagnosed via a blood test and urine test. Estimated glomerular filtration rate (eGFR) provides a measure of how well the kidneys are working and is determined by assessing the amount of creatinine in the blood [6]. Creatinine is a metabolic by-product that is removed by healthy kidneys, but it can build up in the blood as kidney function declines [6]. Additionally, most proteins are too large to pass through the glomeruli; therefore, the presence of protein in urine (called proteinuria) is another indicator of CKD and can be measured using a ‘dipstick’ urine test [6].
How is CKD classified?
CKD is classified into five stages, depending on the level of remaining kidney function and/or the presence of kidney damage. The first two stages are characterised by a normal (or near normal) eGFR, with some signs of kidney damage. From Stage 3 onwards, CKD is classified according to the decline in eGFR; the lower the eGFR, the further the kidney disease has progressed [9]:

| Stages of CKD9 | eGFR (mL/min/1.73 m²) | % of normal kidney function |
| Stage 1: Normal kidney function with some signs of kidney damage | Above 90 | 90%–100% |
| Stage 2: Mild drop in kidney function with signs of kidney damage | 89–60 | 89%–60% |
| Stage 3a: Mild to moderate drop in kidney function | 59–45 | 59%–45% |
| Stage 3b: Moderate to severe drop in kidney function | 44–30 | 44%–30% |
| Stage 4: Severe drop in kidney function | 29–15 | 29%–15% |
| Stage 5: Kidney failure | Below 15 | Less than 15% |
How is CKD treated?
Treatment of early-stage CKD primarily focuses on slowing progression, treating the underlying cause of the disease (if known), managing the risk of cardiovascular disease, and relieving any symptoms [6]. Stage 5 CKD (also referred to as kidney failure) requires renal replacement therapy [6].
Healthy lifestyle behaviours, such as not smoking, eating a healthy diet, and participating in regular exercise are important for maintaining kidney function and managing other health conditions that damage the kidneys (e.g. hypertension and diabetes) [3]. Additionally, certain over-the-counter medicines (such as NSAIDs) can exacerbate CKD and should be avoided [3, 6].
Patients may also require medication to help control blood pressure (e.g. angiotensin-converting enzyme inhibitors or angiotensin-receptor blockers) and blood sugar levels (e.g. sodium-glucose cotransporter-2 [SGLT2] inhibitors) [6].
Renal replacement therapy is typically initiated when eGFR falls below 10%–15% (Stage 5); treatment options include dialysis (either haemodialysis or peritoneal dialysis) or a kidney transplant [10].
Eight golden rules
CKD affects millions of people worldwide. The underlying causes are complex and there are many treatment options available. With this in mind, the organisers of WKD have provided eight golden rules to remember for maintaining kidney health [11]:

For more information on WKD and to find out how you can get involved, visit https://www.worldkidneyday.org/.
The information in this article is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. All content is for general information purposes only. Always seek the guidance of your doctor or other qualified healthcare professional with any questions you may have regarding your health or medical condition.
References
- World Kidney Day. World Kidney Day. Available at: https://www.worldkidneyday.org/about/world-kidney-day/. Accessed March 2022.
- World Kidney Day. 2022 WKD theme. Available at: https://www.worldkidneyday.org/2022-campaign/2022-wkd-theme/. Accessed March 2022.
- National Health Service. Overview: Chronic kidney disease. Available at: https://www.nhs.uk/conditions/kidney-disease/. Accessed March 2022.
- Kidney Care UK. Facts and stats. Available at: https://www.kidneycareuk.org/news-and-campaigns/facts-and-stats/. Accessed March 2022.
- National Institute of Diabetes and Digestive and Kidney Diseases. What is chronic kidney disease? Available at: https://www.niddk.nih.gov/health-information/kidney-disease/chronic-kidney-disease-ckd/what-is-chronic-kidney-disease. Accessed March 2022.
- Chronic kidney disease. Available at: https://patient.info/kidney-urinary-tract/chronic-kidney-disease-leaflet. Accessed March 2022.
- Mayo Clinic. Diabetic nephropathy (kidney disease). Available at: https://www.mayoclinic.org/diseases-conditions/diabetic-nephropathy/symptoms-causes/syc-20354556. Accessed March 2022.
- MSD Manual Consumer Version. Urinary tract obstruction. Available at: https://www.msdmanuals.com/en-gb/home/kidney-and-urinary-tract-disorders/obstruction-of-the-urinary-tract/urinary-tract-obstruction. Accessed March 2022.
- National Kidney Foundation. Estimated glomerular filtration rate (eGFR). Available at: https://www.kidney.org/atoz/content/gfr. Accessed March 2022.
- National Institute for Health and Care Excellence. Chronic kidney disease: Assessment and management. NICE guideline (NG203); November 2021. Available at: https://www.nice.org.uk/guidance/ng203/. Accessed March 2022.
- World Kidney Day. 8 golden rules. Available at: https://www.worldkidneyday.org/facts/take-care-of-your-kidneys/8-golden-rules/. Accessed March 2022.
 Author: Tom O’Sullivan, PhD | Medical Writer | Porterhouse Medical
Author: Tom O’Sullivan, PhD | Medical Writer | Porterhouse Medical




 Group
Group